Claims and Appeals
Interstitial Cystitis
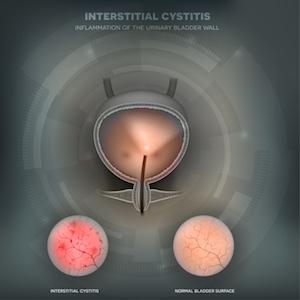
Interstitial cystitis, sometimes called “IC” or “bladder pain syndrome,” is chronic inflammation of the bladder, affecting the walls of the bladder. The exact cause of the interstitial cystitis is unknown. Interstitial cystitis often occurs with persons who have fibromyalgia and irritable bowel syndrome. Interstitial cystitis is incurable.
Symptoms caused by interstitial cystitis include pain in and around the bladder, a frequency or urge to urinate, and pain during sexual intercourse. The test has been developed to affirm whether a person has interstitial cystitis. A cystoscopy can show whether there is bladder wall stiffening (fibrosis); pinpoint bleeding on the bladder wall (diffuse glomerulations); and patches of broken skin (Hunner’s ulcers). However, a positive cystoscopy does not, by itself, establish a diagnosis of interstitial cystitis. Many of the symptoms of interstitial cystitis mirror symptoms caused by other conditions and diseases. For that reason, a diagnosis of interstitial cystitis is made by “ruling out” other possible medical conditions. These other medical conditions include urinary tract infection, sexually transmitted disease and cancer of the bladder to name a few. (Complicating matters for diagnostic purposes is the existence of co-morbidities. For example, a person may have interstitial cystitis and a urinary tract infection at the same time.) In addition to cystoscopy and a “rule out” diagnosis, there must be documentation of symptoms including chronic bladder and pelvic pain; urinary urgency and frequency and other symptoms such as dyspareunia (sexual dysfunction); sleep issues; fatigue (chronic) and tenderness on physical examination in the suprapubic area. Sometimes, laboratory studies may support a diagnosis of interstitial cystitis. For example, urine cultures which do not show bacteria; a positive Parson’s test (a Parson’s test looks for potassium sensitivity) and in APF accumulation in urine (APF means anti-proliferative factor). If a person has depression or anxiety, documented on a mental status examination or a psychological test, the existence of these mental issues can help to establish a diagnosis of interstitial cystitis.
From a Social Security disability perspective, interstitial cystitis is a serious medical condition which can serve as the basis for an award of Social Security disability. For this condition to satisfy the disability requirements, the claimant must establish that her interstitial cystitis rises to the level of a medically determinable impairment. The Social Security “Blue Book” defines a medically determinable impairment as “an impairment that results from anatomical, physiological, or psychological abnormalities that can be shown by medically acceptable clinical and laboratory diagnostic techniques.” (See “Blue Book” Here.) Social Security Ruling 15-1p, makes a licensed medical or osteopathic doctor the only professionals who can diagnose interstitial cystitis is a medically determinable impairment under Social Security’s rules. That diagnosis must be supported by chart notes which document symptoms normally found in patients with interstitial cystitis together with appropriate laboratory findings and medical signs.
Once a diagnosis of interstitial cystitis is determined to be a medically determinable impairment (step 2) of the sequential evaluation process), Social Security proceeds through the remaining steps of the process to determine whether that person qualifies for Social Security disability. Since interstitial cystitis is not a listed impairment, the claimant cannot qualify for disability at step 3. Therefore, Social Security must determine the residual functional capacity of the claimant (that is, what is the most that person can do given the diagnosis of interstitial cystitis). After determining the claimant’s residual functional capacity, Social Security then must decide at step 4, whether that individual can return to her past relevant work (that is the work that she has done in the last 15 years). If the person cannot return to her past relevant work, then Social Security proceeds to step 5 to determine whether a person can perform and adjust to any other work that exists in significant numbers in several regions throughout the United States.
In many cases, persons with interstitial cystitis are required to use the restroom much more frequently than persons without interstitial cystitis. In severe cases, it can be 30 to 60 times a day. Documenting the date and time of needed restroom breaks is important. An easy way to document restroom breaks is to keep a journal. This journal may be helpful not only in proving restrictions from a disability standpoint but also in treating the medical condition itself. The person should give the journal to both the physician treating the condition as well as the attorney representing the person for disability.







